
Mental health 1/2: what your body is also trying to tell you
Stress, anxiety, fatigue, sleep: understanding why mental health is important
Table of contents
This article, we're addressing a topic that affects a huge portion of the population and deserves its place in our conversations about health: mental health.
According to the WHO, nearly 1 in 7 people worldwide lives with a mental disorder, that's over one billion people. Depressive and anxiety disorders are the most common conditions.
And yet, many people still minimize what they're feeling.
We tell ourselves: "It's nothing, it will pass." We wait. We feel guilty. We compare ourselves.
But mental health is not "just in your head."
It also involves the body: sleep, stress, the nervous system, inflammation, metabolic health, and sometimes nutritional deficiencies. Mental health is not separate from the rest of our physiology.
In this article, we'll help you better understand what may be at play when you feel stressed, anxious, irritable, or simply exhausted.
In the second particle of this serie, we'll explore what's useful to observe and adjust to better support yourself.
Shall we begin?
What "mental health" really means
Mental health is not simply the absence of disorder.
EN_Newsleter_MentalHealth_#103.png
It's a state of well-being that allows us to cope with daily stress, function in our lives, mobilize our resources, and navigate difficult periods with a baseline of stability.
EN_Newsleter_MentalHealth_#102.png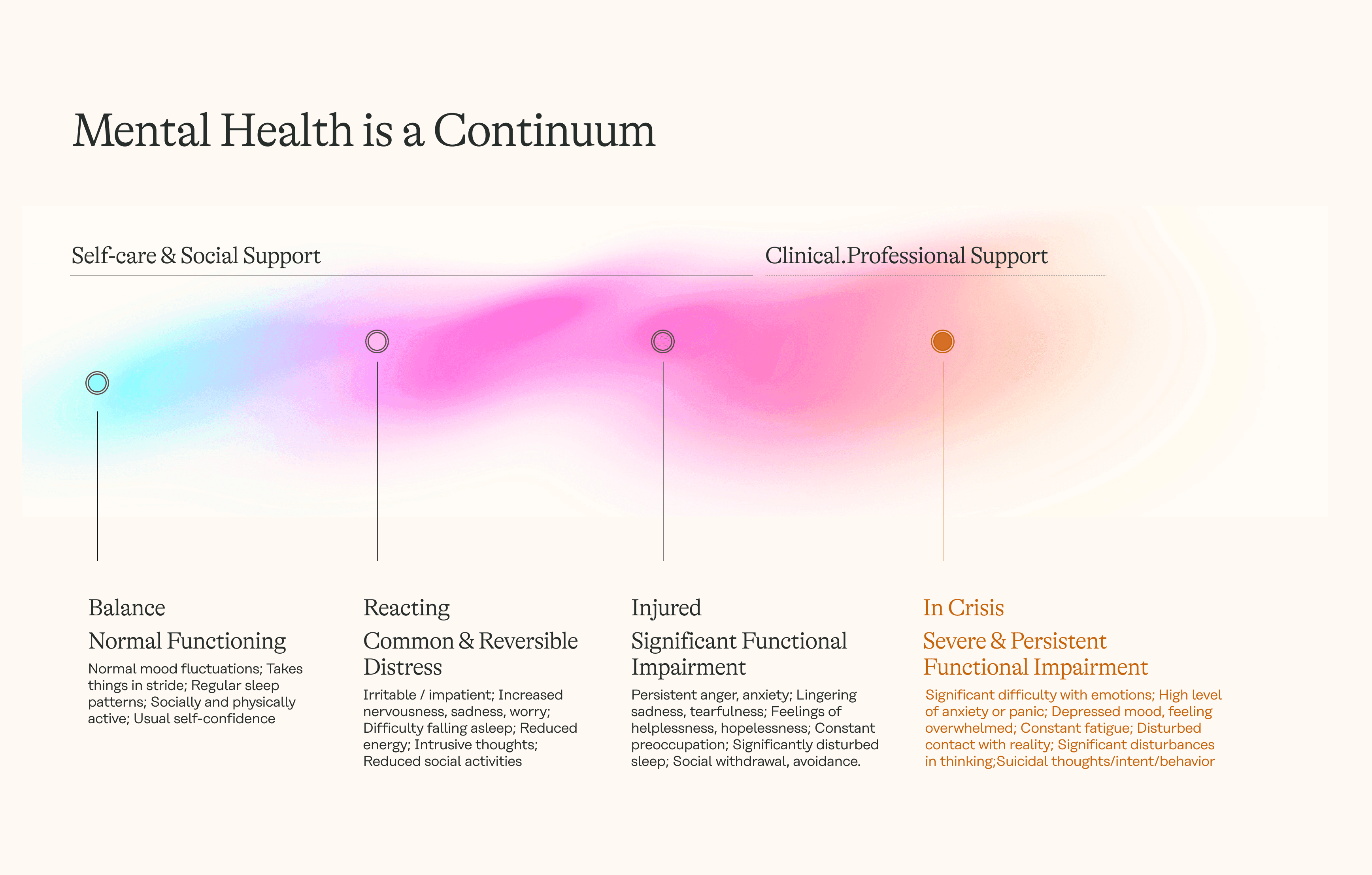
Mental health exists on a continuum.
We're not either "well" or "unwell". Our balance evolves according to our context, biology, environment, lifestyle habits, relationships, and the events we experience.
Understanding this is already a step toward leaving judgment behind.
The most common states
Depression
It can manifest as persistent sadness, loss of interest, deep fatigue, sleep disturbances, slowing down, difficulty concentrating, and sometimes physical manifestations.
Anxiety
It corresponds to excessive or hard-to-control worry, often associated with muscle tension, irritability, sleep disturbances, palpitations, or a constant sense of being on alert.
Chronic stress
It's not just "having a lot to do." It's a state in which the body remains mobilized for too long, without sufficient recovery. Over time, this can affect sleep, energy, mood, concentration, blood sugar, and overall health.
Key takeaway: These states often have both emotional and physical expressions. The body is fully involved in the experience.
Misconceptions that delay care
"Mental disorders are rare."
False. They're common globally and in France. In France, anxiety disorders and depressive episodes affect a significant portion of the population, with a higher frequency among women.
"Mental health can't be measured."
False. We can:
Assess symptoms with validated clinical questionnaires used by healthcare professionals to track symptom progression and adapt care
Monitor associated biological factors such as inflammation, iron status, vitamin B12, folate, vitamin D, or certain metabolic parameters
Observe daily indicators with connected tools like sleep and sometimes heart rate variability
"Stress is always bad."
False. Acute stress is a normal adaptive response. It can temporarily improve alertness, concentration, or performance. The problem is chronic stress, when the body remains activated without sufficient return to calm. That's when the effects become harmful.
"Therapy is only for severe cases."
False. Psychotherapy can be useful for prevention, during a difficult period, or in the context of a diagnosed disorder. It's not reserved for extreme situations.
The mind-body connection: what's really happening
EN_Newsleter_MentalHealth_#101.png
For a long time, we separated mental health and physical health. Today, research shows close links between mood, stress, inflammation, sleep, metabolism, and gut health.
Some examples:
Glycemic instability and metabolic dysfunction are associated with a higher risk of depressive symptoms.
Low-grade inflammation, particularly via markers like high-sensitivity CRP, is associated with more depressive symptoms in numerous studies.
Sleep directly influences mental health, and its improvement is associated with improved psychological well-being.
The gut-brain axis appears to play an important role via immunity, the vagus nerve, microbial metabolites, and certain neuroendocrine pathways. It's a very active, promising field, but still evolving.
What this changes in practice
Taking care of your mental health isn't just about "thinking differently."
It's also about looking at whether your biological terrain supports or, conversely, undermines your psychological balance:
Sleep quality
Stress load
Inflammatory state
Glycemic balance
Iron, magnesium, B vitamins, vitamin D status
Lifestyle, movement, recovery, social environment
In other words: the brain doesn't function in isolation.
Better understanding what your body is telling you
It's precisely because mental health also has a physiological dimension that it can be better observed.
At Lucis, we analyze over 110 biomarkers to help you better understand certain factors that may influence your energy, stress resilience, and overall functioning.
For example:
For example:
Inflammation markers, such as high-sensitivity C-reactive protein (hs-CRP)
Parameters related to glucose metabolism, such as fasting glucose, fasting insulin, and HbA1c
Certain nutritional status markers, such as vitamin D, vitamin B12, folate, iron/ferritin
And, depending on the context, markers that help better understand the stress response, such as cortisol awakening response.
This data never replaces a psychological or medical evaluation, but it can enrich the understanding of your biological terrain and help build a more integrative approach.
In the second part, we'll explore concrete levers that can help support this balance more precisely.
Share this article with someone who might need it.
Sometimes, understanding what's happening is already a first step toward relief.
Disclaimer
The information contained in this newsletter is provided for educational purposes only and does not constitute medical advice, diagnosis, or treatment. If you are in psychological distress or worried about yourself or someone else, contact a healthcare professional immediately.
Références
Léon C, du Roscoät E, Beck F. Prévalence des épisodes dépressifs en France chez les 18–85 ans : résultats du Baromètre santé 2021. Bulletin Épidémiologique Hebdomadaire. 2023;(2):28–40.
Li Z, et al. A meta-analysis study evaluating the effects of sleep quality improvement on depression and anxiety in adults. 2025.
Loh JS, et al. Microbiota–gut–brain axis and its therapeutic applications. Signal Transduction and Targeted Therapy. 2024.
Santé publique France. Prévalence des états anxieux chez les 18–85 ans : résultats du Baromètre Santé publique France (2017–2021). 2025.
Zhu Z, et al. The microbiota-gut-brain axis in depression. Frontiers in Immunology. 2025.
Written by Anaïs Gautron
More insights, straight to your inbox.
New articles on biomarkers, performance, and wellness — no noise, just substance.
